UVA Health Plan/Pharmacy
Health Plan Communications:
E-Visits
- Non-audiovisual, non-telephonic online communication, and telephonic coverage with medical providers are not covered by the UVA Health Plan. These include E-visits which are online visits with providers using MyChart. If billed, you are responsible for the full cost of the service, and the cost will not be applied towards deductibles or out-of-pocket maximums. For additional information regarding UVA Health MyChart E-Visits visit the FAQ page.
Consolidated Appropriations Act (CAA) / No Surprises Act (NSA)
Signed into law on December 27, 2020, the $900 billion COVID-19 stimulus package provides funding for COVID-19 testing and tracing, vaccine distribution, and temporarily increases unemployment benefits The package also includes Transparency in Coverage machine-readable file requirements for in-network negotiated rates and out-of-network allowed amounts and billed charges. The link to the machine-readable file will by posted by July 1, 2022 to the UVA Health Plan’s microsite at https://www.aetnaresource.com/p/UVA-Health-Plan.
Your medical, dental, and/or vision benefits can begin on the first date of employment for most new hires* (or choose to wait until the first of the month if you have coverage elsewhere).
- Date of employment: If you need coverage immediately, you have the option to start your medical, dental, and/or vision benefits as of your date of employment. This may be a good option if you are currently not covered elsewhere, or you desire coverage as soon as possible.
- *When enrolling in benefits due to a UVA “change job” or “transfer," coverage begins on the first of the month following the event date. If the event date is on the first of the month, coverage begins immediately.
- First of the month following your date of employment: You can choose to start your medical, dental, and/or vision benefits on the first of the month after you are hired. This may be a good option if you have coverage from a previous employer or are under a family member’s coverage that is still active through the end of the month. However, if you are hired on the first of the month, your benefits coverage begins on your first date of employment; you cannot start coverage the following month.
- No medical, dental, and/or vision coverage: You can officially waive your medical, dental, and/or vision benefit options as well as enroll or waive in other benefits during your new hire change benefit event.
Please review the Coordination of Benefits document regarding your coverage and how it works with your prior employer.
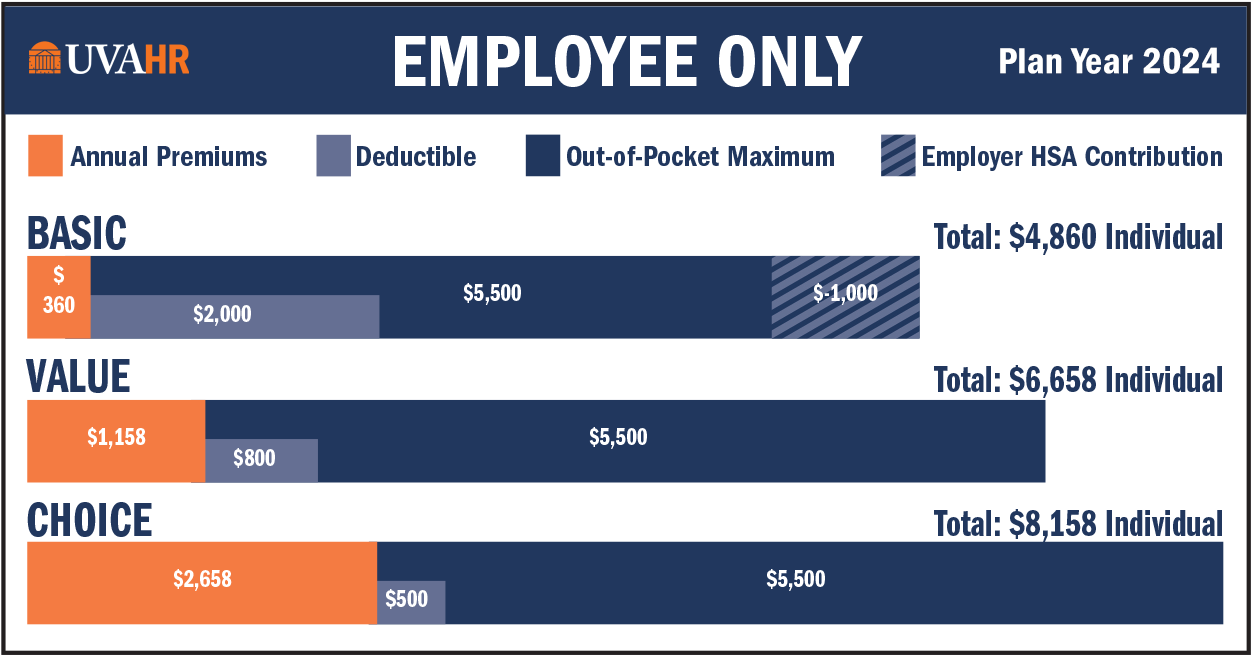
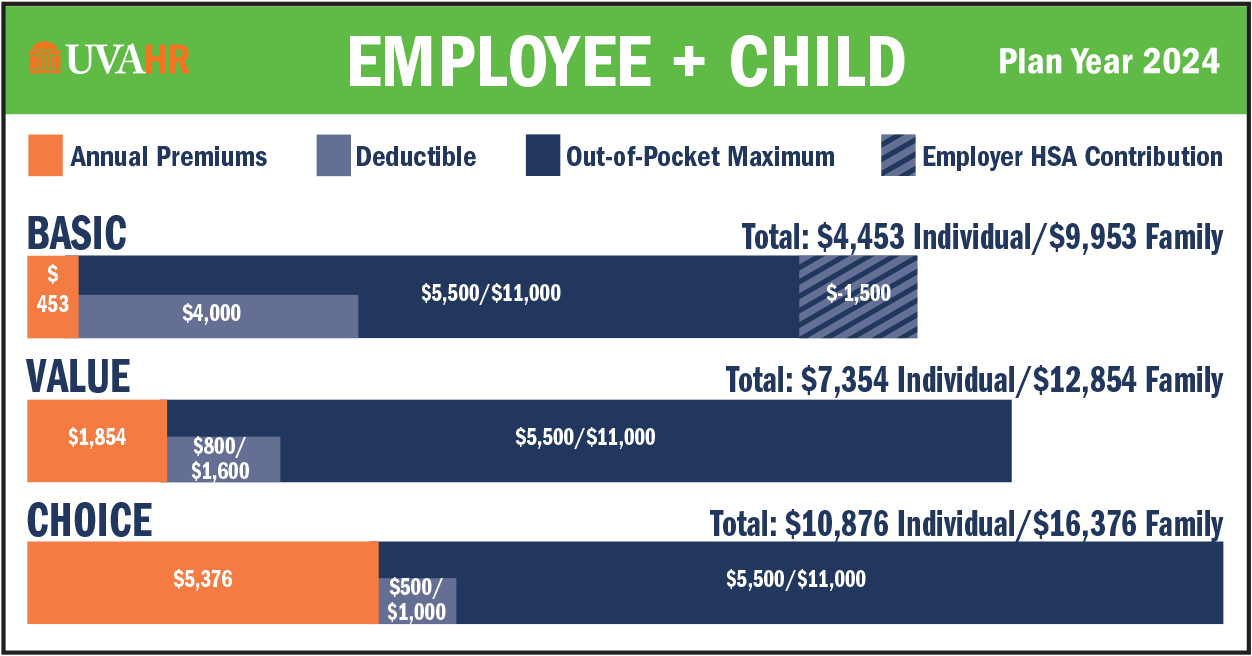
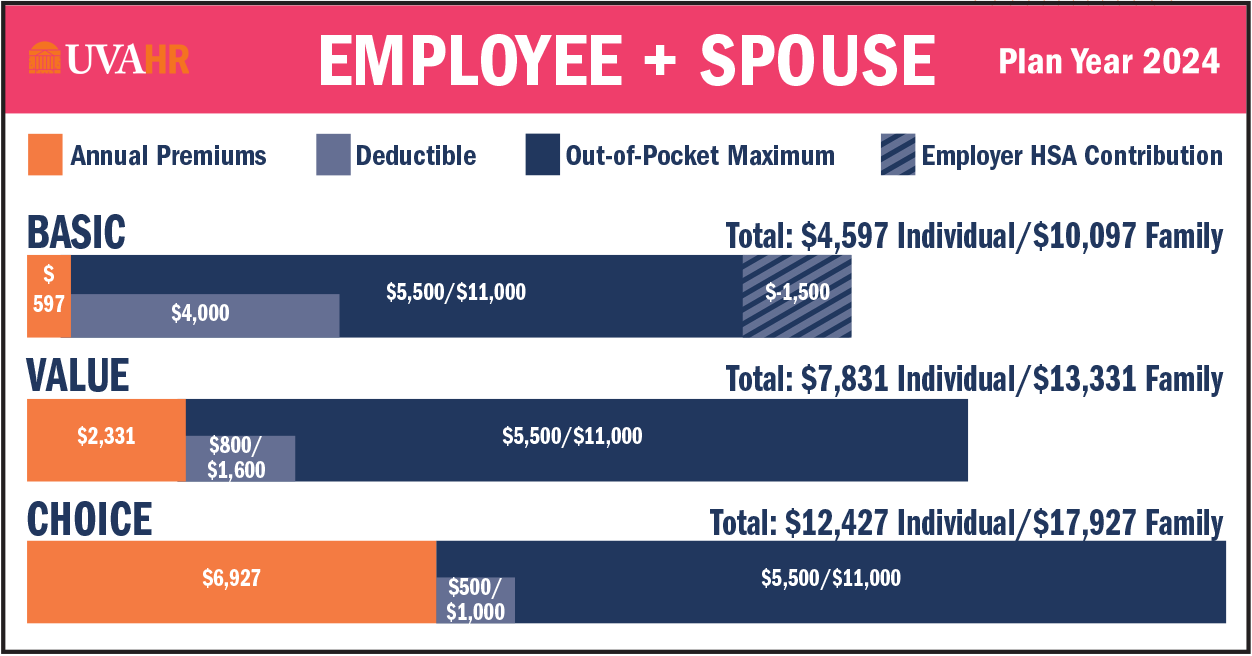
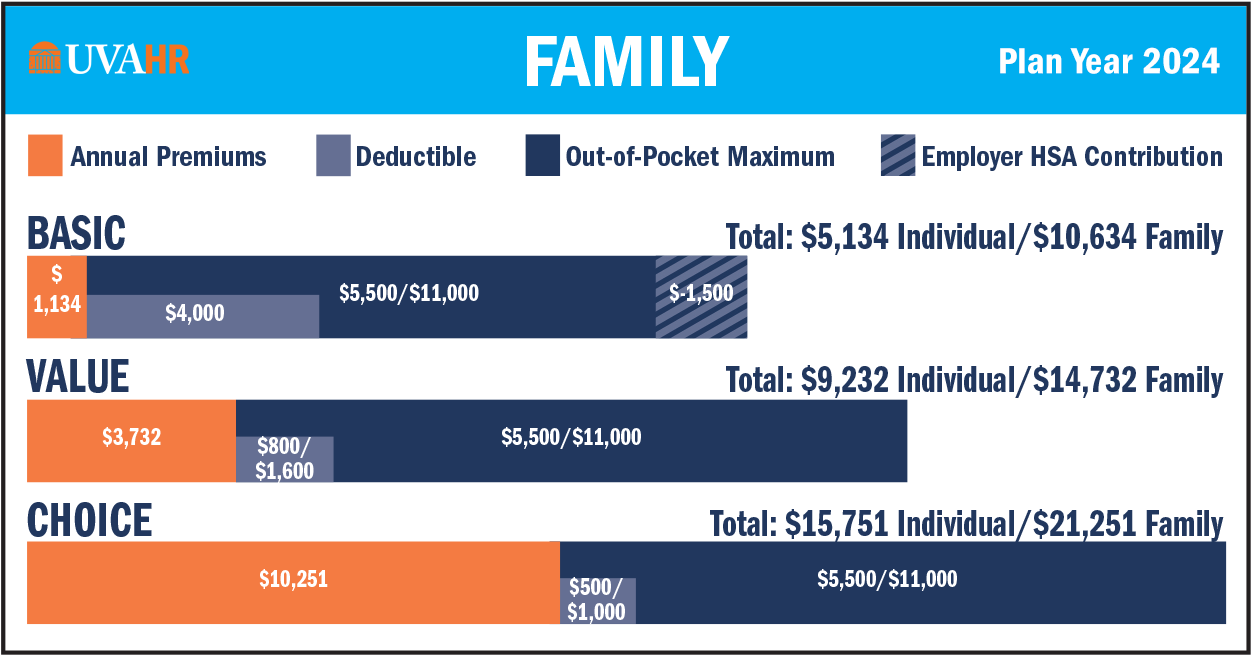
Every UVA employee has different benefits needs, and you have 3 health plan options to choose from to meet your needs. All options are administered by Aetna:
- Basic Health (high deductible)
- Value Health
- Choice Health
NEW: Enjoy these NEW personal video stories that explain why each of the HR team members chose the health plan option they did during Open Enrollment: